What is Telemedicine? What is the difference between Telehealth?
It is said that medical treatment is better made face to face. However, the sad fact is that many people residing in rural areas can not seek medical treatment in person because they live too far from a health care provider. Telehealth video conferencing solutions allow doctors and patients to meet from wherever they may be with no need for travel for appointments.
Health professionals have also developed this technology to meet distant patients living in rural areas. But over time, the larger picture was seen by medical professionals and the U.S. government. The opportunity to meet metropolitan areas with healthcare problems and adapt to health treatment by exchanging medical services and patient health information was realized.

What is Telemedicine?
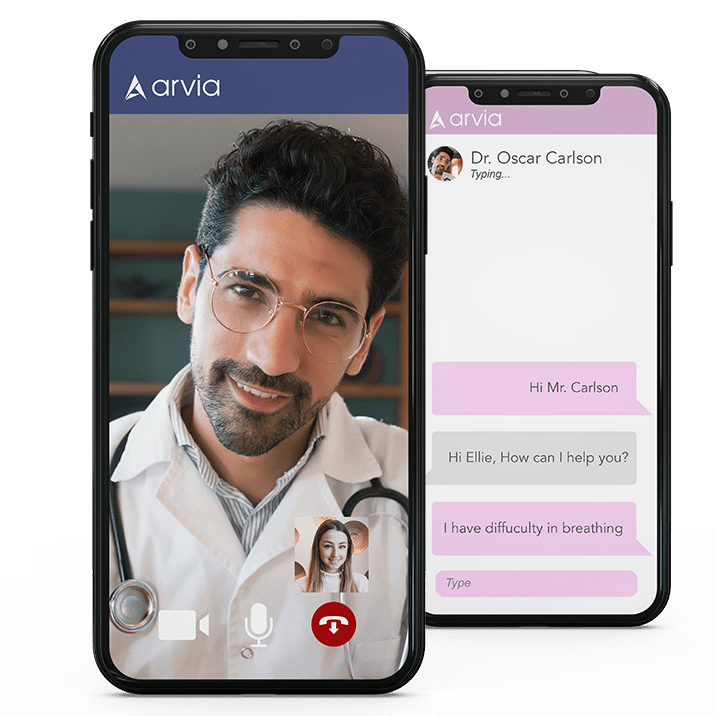
The World Health Organization (WHO) calls telemedicine a “remote treatment.” It’s using telecommunications technologies and information systems to provide patients with remote health services. Doctors use telemedicine for image delivery, video appointments, and remote medical diagnosis.
Today, people are no longer expected to schedule an in-person appointment to seek care with a specialist. Using safe video and audio links enables doctors to treat people who live in areas with restricted access to treatment.
What is Telehealth?
“The utilization of electronic information and telecommunications technologies to support and promote long-distance clinical health care, patient and professional health education, public health and health administration.” is a definition for telehealth by HealthIT.gov.
Although this concept looks a lot like telemedicine, the difference is significant. In contrast to telemedicine, telehealth also covers non-clinical events such as administrative meetings, continuing medical education, and training for doctors. Telehealth is not a particular service but a collection of methods for improving the delivery of patient care and education.
In general, telehealth can be viewed as a holistic term because telemedicine and telecare are part of it.
Telemedicine and Telehealth
The terms telemedicine and telehealth carry with them much discussion in the field of healthcare among individuals. One explanation for this dispute is because of the different meanings of the words themselves. Most researchers claim that telemedicine is physician-focused and that telehealth involves all health professionals. The two terms are likely to become more separate when technology continues to evolve in the medical industry. However, the differences can be understood by examples:
Telehealth:
- A public health software that warns the public about an outbreak of a disease
- Health education video-conferencing network
Telemedicine:
- A mobile app that lets doctors treat patients remotely through video chat
- A software solution that allows primary care providers to send patient photographs of a rash or mole to a dermatologist for rapid examination at another location

History of Telemedicine
Telemedicine is not a new practice, in contrast to common belief. Indeed the telemedicine concept dates back to the 19th century. What began with a few hospitals in remote areas trying to serve patients became an integrative network across the spectrum of treatment. Telemedicine history will show how we have reached where we are today.
Throughout the Civil War, apart from requesting medical supplies and services, casualties and injuries were reported using the telegraph. It is considered to be one of the first telemedicine innovations adopted.
The “teledactyl” was published in a science magazine by Dr. Hugo Gernsback in 1922. Gernsback predicted that this sensory feedback system would allow physicians to see their patients over a TV screen and touch them with robot arms from miles away.
After this date, developments rapidly increased until today. Many people today have access to simple telemedicine equipment such as mobile phones and computers. Through increased connectivity, individuals can easily communicate with a provider in rural areas and busy urban areas. For example, we now have live video telemedicine technology. Still, most of the U.S. population has experience with online video chat applications (such as Skype or Facetime) and uses a computer or mobile device to use them. Home-use medical devices allow carers to track anything from vital to glucose levels. Doctors will collect crucial medical knowledge and decide without patients going to a doctor’s office to step foot.
In 2026, telemedicine is expected to be an industry worth $175 billion, and an integral part of modern healthcare delivery. Telemedicine history shows we have come so far from where we began, and yet there is still a long way to go.
Conclusion
Initially, telemedicine was developed to treat patients in remote regions, far from local health centers, or in places where medical providers were in short supply. Although telemedicine is still being used to solve these problems today, it is increasingly becoming a tool for efficient medical care. The linked patient today needs to spend less time in the doctor’s waiting room, and get prompt treatment when they need it for minor yet urgent conditions.
Combined with the unavailability of many overburdened medical professionals, this demand for more convenient treatment has led to the rise of telemedicine companies. Most give patients access to medical treatment 24/7 via an on-call physician paid by the organization. Others provide access to extra clinical personnel and specialists to hospitals and more extensive health centers to outsource individual cases. Some also have a telemedicine network that doctors can use to give their patients virtual visits.
Telemedicine is rapidly becoming a way to give medical practices an advantage in a dynamic healthcare environment where remaining independent or sustaining a healthy bottom line is hard.